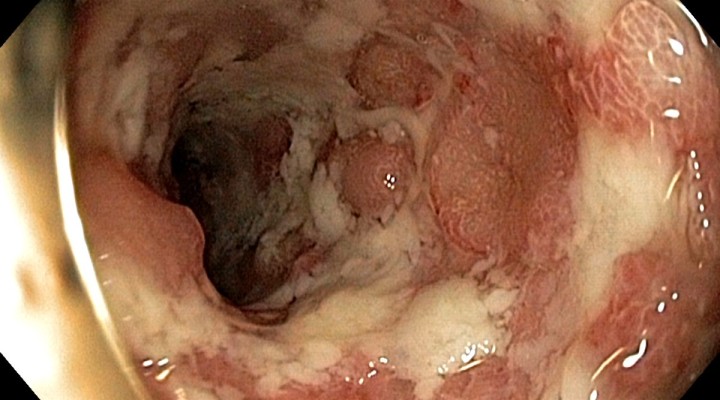
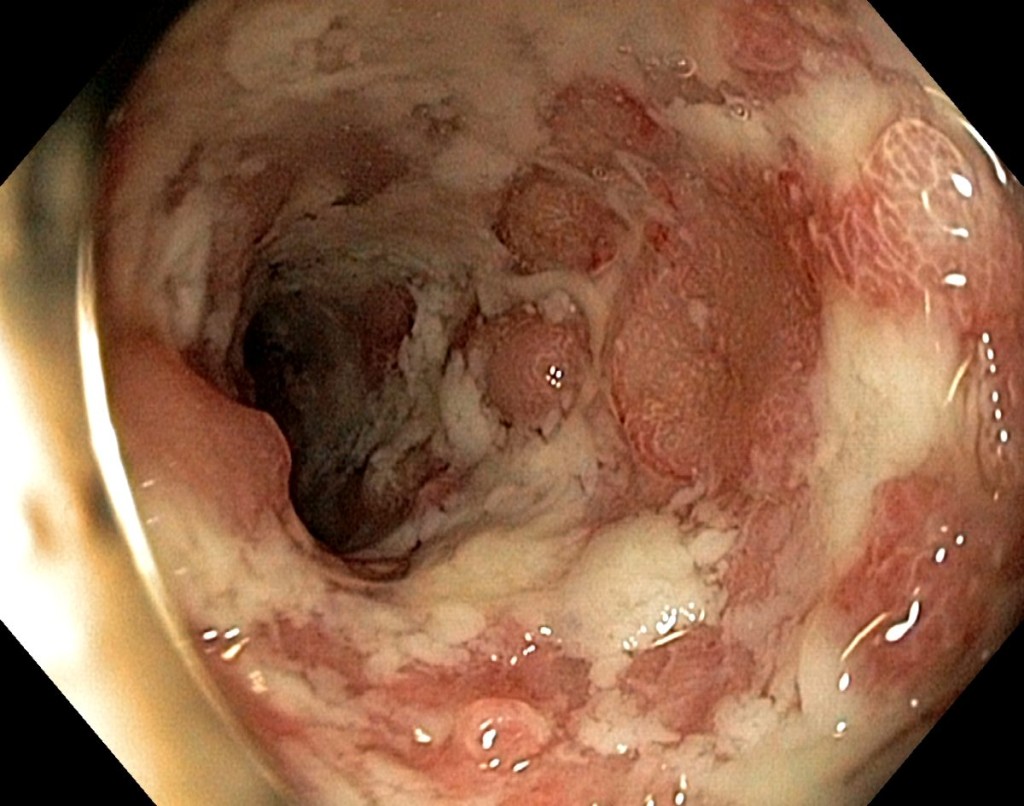
- Put patient on NPO status (nothing by mouth) for bowel rest (especially if bowel perforation is suspected)
- Start IV fluids to maintain hydration and electrolytes
- Advise patient to limit activity
- Monitor bowel sounds
- Monitor vital signs
- Completion of an early warning assessment tool, such as the modified early warning score (MEWS), should be performed and followed as per hospital policy.
- Monitor for signs and symptoms of infection (peritonitis)
- Monitor for signs and symptoms of hemorrhage (caused by ulcers).
- As diet advances, place on a low fiber, high protein diet
- Avoid the following foods: nuts, alcohol, caffeine
- Other documentation should be implemented and completed, including a food chart if there is concern regarding nutritional status and a fluid balance chart where intravenous fluid is administered, or where there is concern regarding fluid intake or urine output. Fluid balance charts are an important part of hydration monitoring.
- Instruct patient on smoking cessation
- Provide emotional support. Emotional support is vital and is an important aspect of holistic care provision.
- Teach the patient about the disease process and the typical treatment regimen. Areas to include in the teaching plan include the signs of disease complications, the importance of rest and stress reduction, and any dietary adjustments.
If the patient requires surgery, several nursing interventions are important in the preoperative phase:
- First, conduct preoperative teaching sessions on deep-breathing techniques and leg exercises.
- Discuss the operative procedure and the typical postoperative course.
- When appropriate, discuss with the patient information on stoma placement and stoma care.
- After surgery, ensure a healthy respiratory status for the patient by encouraging the patient to cough and deep-breathe every 1 to 2 hours.
- Manage patient pain and discomfort with prescribed analgesics and proper positioning techniques.
- Monitor for adequate wound healing by checking the color and approximation of the wound and noting any wound drainage or odor.
- Note the stoma size and color during every shift and immediately report any duskiness noted at the stoma site.
- Note the condition of the skin around the stoma; protect the skin with appropriate barrier products because ileostomy drainage is extremely caustic to skin tissues.
- Encourage the patient’s participation in ostomy care.
- Assess whether a community resource person from the United Ostomy Association is needed to offer the patient additional support.