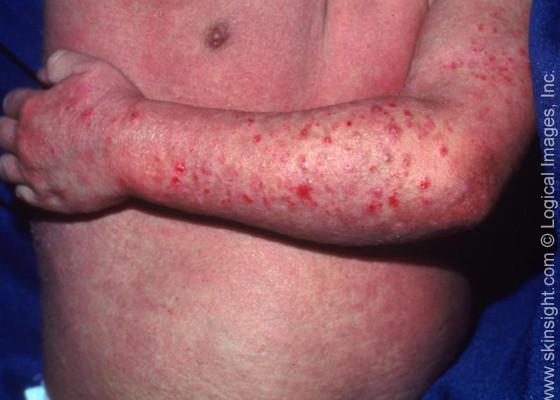
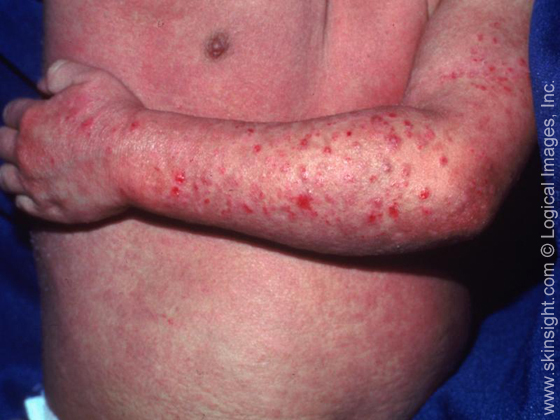
- Assess skin, noting color, moisture, texture, temperature; note erythema, edema, tenderness since specific types of dermatitis may have characteristic patterns of skin changes and lesions.
- Assess the skin systematically. Look for areas of irritant and allergic contact. Flexural areas (elbows, neck, posterior knees) are common areas affected in atopic dermatitis.
- Assess skin for lesions. Note presence of excoriations, erosions, fissures, or thickening. Open skin lesions increase the patient’s risk for infection. Thickening occurs in response to chronic scratching (lichenification).
- Encourage the patient to adopt skin care routines to decrease skin irritation since one of the first steps in the management of dermatitis is promoting healthy skin and healing of skin lesions.
- Bathe or shower using lukewarm water and mild soap or non-soap cleansers. Long bathing or showering in hot water causes drying of the skin and can aggravate itching through vasodilation.
- After bathing, allow the skin to air dry or gently pat the skin dry. Avoid rubbing or brisk drying since they can irritate the skin and exacerbate the itch-scratch cycle.
- Apply topical lubricants immediately after bathing.
Lubrication with fragrance-free creams or ointments serves as a barrier to prevent further drying of the skin through evaporation. Moisturizing is the cornerstone of treatment. Over-the-counter moisturizing lotions include Eucerin, Lubriderm, and Nivea. Lotions are lighter and less emollient than creams. If more moisturizing is required than a lotion can provide, a cream is recommended. These include Keri cream, Cetaphil cream, Eucerin cream, and Neutrogena Norwegian formula. Ointments are the most emollient. Vaseline Pyre Petroleum Jelly or Aquaphor Natural Healing Ointment may be beneficial.
- Apply topical steroid creams or ointments.
These drugs reduce inflammation and promote healing of the skin. The patient may begin using over-the-counter hydrocortisone preparations. If these are not effective, the physician may include prescription corticosteroids for topical use. Usual application is twice daily, thinly and sparingly. Do not use with an occlusive dressing, because this potentiates the action and systemic absorption of the steroid. Usual duration of use of topical steroids is up to 14 days in adults.
- Use cool compresses on pruritic areas of the skin as cool, moist compresses help relieve pruritus and itching. Additionally, cool baths with colloidal oatmeal (e.g., Aveeno) can provide relief.
- Apply topical immunomodulators (TIMs):
- Tacrolimus (Protopic)
- Pimecrolimus (Elidel)
Tacrolimus (Protopic) has recently been approved for the treatment of atopic dermatitis. TIMs alter the reactivity of cell-surface immunological responsiveness to relieve redness and itching. In 2005, the Food and Drug Administration advised a potential cancer risk with long-term use of pimecrolimus and tacrolimus based on animal studies.
- Prepare the patient for phototherapy or photochemotherapy since this treatment modality uses ultraviolet A or B light waves to promote healing of the skin. The addition of psoralen, which increases the skin’s sensitivity to light, may benefit patients who do not respond to phototherapy alone.
- Encourage the patient to avoid aggravating factors. Some change in lifestyle may be indicated to reduce triggers.
- Allow patients to verbalize feelings regarding their skin condition and assist in identifying ways to enhance their appearance.
Sources:
https://nurseslabs.com/dermatitis-nursing-care-plans/
https://nursing88.blogspot.com/2010/09/nursing-care-plan-ncp-eczema.html