Kayla is not feeling well. This afternoon, after taking a nap, she woke up with a fever and body weakness. She heads to the kitchen to get herself a glass of water as she encounters her sister, Elaine, who just arrived from hospital duty.
After telling Elaine about how she was feeling, Elaine rushes to get her sphygmomanometer and stethoscope.
“I’m going to perform a tourniquet test on you,” Elaine says.
“What? Why?” Kayla asks.
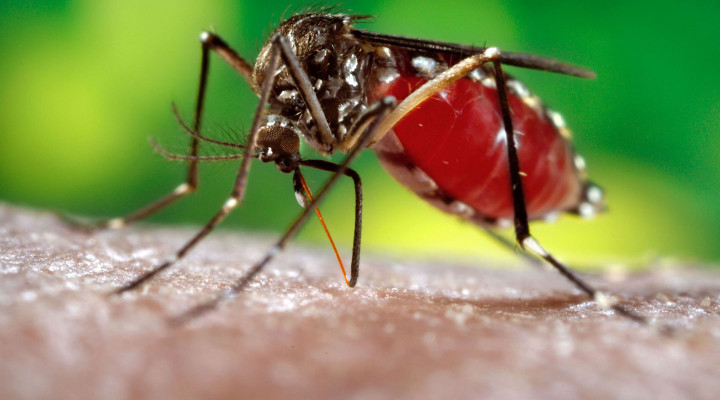
“There has been an increased number of Dengue cases in the hospital these days. This is to see if you are one of them or not.”
“Oh, please don’t let this be dengue,” Kayla thinks to herself as she imagines possible blood tests and blood transfusions she will be getting if she gets admitted.
Tourniquet test: An overview
The tourniquet test is considered as an important basic screening test for dengue. The World Health Organization (WHO) also suggests using the tourniquet test as a vital parameter in the diagnosis of dengue. Due to limited resources in highly rural areas in endemic countries, this test is helpful in the diagnosis and indication of dengue infection.
In this test, the blood capillaries are examined for their ability to withstand increased pressure, giving a good indication for assessing the blood vessel and whether it will lead to Dengue Shock Syndroe or Dengue Hemorrhagic Fever. Here, petechiae is checked of those small red spots under the surface of the skin, which are formed when blood leaks from capillaries into the skin.
How to perform the Tourniquet test
- Measure the blood pressure
- Pump up a blood pressure cuff on one of the arm to the pressure halfway between the diastolic and systolic blood pressure
- Keep it for 5 minutes and then ease the pressure
- Examine the extremity of the pressure of petechiae
- The number of petechiae within a circumscribed area of the skin may be counted, or the results may be reported in a range from negative (no petechiae) to +4 positive (confluent petechiae).
- The tourniquet test can be negative especially early in the disease or in obese patients or in patients with shock
However, this test is not considered to be completely reliable for confirming dengue as there are certain factors that can influence the results such as premenstrual and postmenstrual period in women and sun damaged skin in people. These people are sure to have relatively fragile capillaries. On the other hand, it can come in useful in monitoring a patient’s condition when he is suffering from Dengue Shock Syndrome or Dengue Hemorrhagic Fever.
Sources:
- https://www.medscape.com/viewarticle/725639_3
- https://medical-dictionary.thefreedictionary.com/tourniquet+test
- https://www.onlymyhealth.com/how-do-tourniquet-test-dengue-1301899878
- https://www.who.int/csr/don/archive/disease/dengue_fever/dengue.pdf