Tessie tears a bit after reading a tear-jerking chapter from the book she’s currently obsessed with. Why on earth should her favorite character die because of lung cancer? Aren’t there any treatments that could cure lung cancer? Would’ve she gotten better? She scolds herself for being too emotional and too attached to the story. As she closes the book, she still couldn’t stop thinking if there really is something that can be done in order to address cancer.
Cancer kills about 8 million people yearly and is challenging to treat, let alone cure. Immune checkpoint inhibitors have permitted physicians to make meaningfully more progress against advanced cancer than they’ve accomplished in decades. Combined with traditional chemotherapy and radiation treatment, the novel drugs enhance the immune system and offer major, long-term cancer remissions for patients with metastatic melanoma. Additionally, there is growing evidence that they can work on other types of malignancies.
Getting to know checkpoint inhibitors
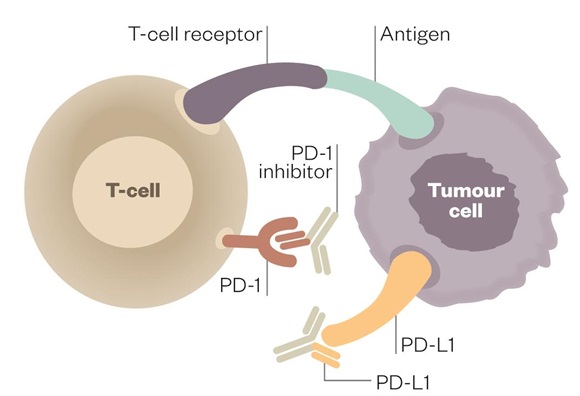
 Immunotherapy includes numerous different treatment approaches, each of which has a diverse mechanism of action, and all of which are intended to boost or reestablish immune function in some manner. One of them are checkpoint inhibitors or immunological brakes” which allow the immune system to avoid overactivation of the immune system on healthy cells.
Immunotherapy includes numerous different treatment approaches, each of which has a diverse mechanism of action, and all of which are intended to boost or reestablish immune function in some manner. One of them are checkpoint inhibitors or immunological brakes” which allow the immune system to avoid overactivation of the immune system on healthy cells.
CTLA-4 has been shown to be perversely upregulated and present on the surface of T cells in certain cancers, diminishing T-cell activation in response to tumor cells. PD-1 is another immunologic checkpoint that has been found to be upregulated in certain tumors; it hinders T-cell function contributing to the tumor’s ability to evade the immune system.
How they work
Inhibiting a checkpoint or in other terms, “releasing the brakes” on the immune system may enhance the anti-tumor T-cell response. This class of therapy has shown efficacy in cancer and clinical trials are ongoing.
According to Louis Weiner, an immunotherapy expert and gastrointestinal oncologist at Georgetown University in Washington, DC, “PD-1/PD-L1 inhibitors look important across a pretty wide swathe of cancers. What got people excited was a lesser [compared with melanoma] but still significant response rate in non-small-cell lung cancer (NSCLC), as well as in bladder, and head and neck cancers.”
Unlike other conventional therapies
PD-1 and PD-L1 inhibitors have been said to induce a higher response rate across a wider range of tumors than other immunotherapies. Out of all of the therapies established to harness the power of the immune system to fight cancer over the past several decades, PD-1/PD-L1 inhibitors look to be the most promising, even though it is still relatively early days in their development.
Furthermore, compared to other immunotherapies in terms of the numbers of cancer patients who respond to them across a number of different tumor types, PD-1/PD-L1 inhibitors also seem to lead compared with standard therapy in terms of their duration of response, although so far follow-up of trials has been at most a few years.
While the checkpoint inhibitors tested thus far have produced some notable results, the drugs are not effective in all patients. Efforts at refining response rates led logically to combinations of more than one checkpoint inhibitor such as combinations of CTLA-4 and PD-1 inhibitors, which at present, are in phase I and II clinical trials for treating various cancers.
According to Drs. Tannir, an associate professor in and deputy chair of the Department of Genitourinary Medical Oncology and Sharma, an associate professor in the Department of Genitourinary Medical Oncology, they are anticipating that checkpoint inhibition will be one of the leading prototypes in cancer research over the next several years, as investigators try numerous combinations and treatments to determine the optimum treatment for specific patient populations.
Sources:
- https://health.clevelandclinic.org/2014/10/top-10-medical-innovations-for-2015/
- https://www.fightcancerwithimmunotherapy.com/ImmunotherapyAndCancer/TypesOfCancerImmunotherapy.aspx
- https://www.pharmaceutical-journal.com/news-and-analysis/features/immune-checkpoint-inhibitors-bring-new-hope-to-cancer-patients/20067127.article
- https://www.mdanderson.org/publications/oncolog/previous-issues/2014-august/immune-checkpoint-inhibitors-show-promise-against-metastatic-renal-cell-carcinoma-other-difficult-to-treat-cancers-oncolog-august-2014.html